Article series
Experiences and case reports by Prof. Tietz, Director of the Institute for Fungal Diseases
04.07.2022
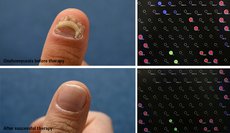
The hands of the guitarist
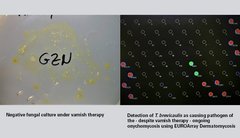
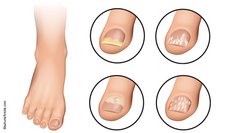
According to a survey conducted by YouGov only a quarter of patients with recurrent foot mycosis know that they are contagious for others and can also spread the infections to other body parts. The rock guitarist who presented with toenail mycosis [...] was also unaware that the pathogen, which was still in his untreated feet, had now spread to the thumbnail and fingernails of his active hand.
27.06.2022
A shocking case
I recently received the following letter from a family from L.:
Our 6-year-old spends a lot of time on his grandparents’ professional farm. While there, he hit his head. The resulting wound developed into a suppurative patch. Our son then received three operations by paediatric surgeons. The dermatological department at the hospital also looked at his case and diagnosed him with pyoderma gangraenosum. He was then treated with cortisone and antibiotics but new patches developed on his head.
25.04.2022
Dermatological mail-in PCR laboratories
I often receive questions from dermatologists describing events in their mycological mail-in laboratory. In my opinion, the establishment of local laboratory collectives is an excellent development. It’s a brilliant idea that pools strengths and is good for everyone, both colleagues and patients.
14.02.2022
Of wrestling mats and hair salons
Mycoses spring in every nook and cranny. It is not only a recent phenomenon that patients get a fungal infection with their haircut, but since the easing of the COVID restrictions in this sector, the golden and silver combs are particularly busy again.
12.01.2022
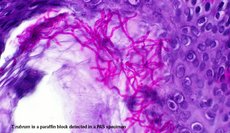
The beacons of dermatology
Fungal cultures and their aesthetically pleasing structures will always hold a special place in my heart, but even I must admit that the introduction of PCR into mycological diagnostics was revolutionary. I have been even more impressed and convinced in recent years by the possibilities of gene-based mycological diagnostics for both diagnosis and therapy.
10.09.2021
Corona is giving a boost to mycology
Recently, a patient said goodbye to me with the words: “If we are not successful with the culture, then I want the genetic test. My health insurance company agreed to pay for it”. This sounded like a declaration of war by the 75-year-old to the fungus. A lady of the same age told us: “I have not been able to do my favourite thing lately, travelling. For that I can now afford a PCR for my nails”. A 16-year-old appeared with the following wish: “It’s not a fungus, my doctor thinks it’s a fungus. I would like to clarify this by PCR “.
11.08.2021
A gift from the heavens
“The Times They Are a-Changin” is one of the best known songs from Bob Dylan, a winner of the Nobel Prize for Literature. As frequently acknowledged, the same applies for the venerable mycology, which is getting more and more interesting. Another example of an until recently unknown pathogen is Trichophyton indotineae. Its nomenclature seems not yet concluded. In this respect mycology unfortunately keeps changing all too often, which is also the case with other pathogens.
17.06.2021
A well-travelled fungus
This pathogen’s discovery was a complete coincidence. In 1989, I had a teaching assignment at the medical faculty in Luanda, where I was supposed to teach medical students, but ended up learning more than teaching, of malaria, cholera, tetanus neonatorum and the people suffering from all these diseases. During examinations of patients with acute vaginal mycosis at a women’s clinic, we found a pathogen that did not fit into any identification system known up to that date. It was lacking chlamydospores, which are typical for C. albicans. Its biochemical structure was not to be found in any detection system, either. And still isn’t today.
17.06.2021
New variants and mutations
One hot-button word is still going round: Mutations. However, we are not talking of viruses. Also fungi develop in an evolutionary process. These may not be as flexible as most viruses and bacteria from a genetic perspective, but they are often much smarter. This is because their strategy is almost always based on an arrangement with the immune system.
19.04.2021
Fungi in Lockdown
The word Corona is still on everyone’s lips. In the wake of the virus, however, other pathogens are also spreading. Some benefit from the pandemic, among them the fungal pathogens. Prime examples of the increase in mycoses are infections with anthropophilic pathogens such as T. rubrum, C. albican, C. auris in COVID-19 patients in the USA and M. furfur, but also zoophilic pathogens such as T. benhamiae, especially in children.
31.03.2021
The accursed clinical eye
According to Professor Hans Rieth, the unforgotten master of mycological entertainment, the clinical eye is often a relative of the evil eye. He described the problem of incorrect visual diagnoses, which still occurs today. Around 30% of patients who go the doctor believing they have a fungal infection, in fact have a non-infectious nail disease.
19.03.2021
A feeling of Sherlock Holmes
The marvellous city of Edinburgh inspired several novelists such as Joanne K. Rowling (“Harry Potter” and Robert Louis Stevenson (“The strange case of Dr Jekyll and Mr Hyde”) to write works of world literature, and the physician Arthur Conan Doyle to create the character of Sherlock Holmes. After introducing PCR testing in our practice laboratory, I felt a bit like Sherlock Holmes myself, like a master detective able to quickly and elegantly solve even the most difficult case.
16.03.2021
Up to the last spore
Professor Seebacher, a leading dermatomycologist, always warned us never to end onychomycosis therapy too early. Here are the reasons: Mycosis does not confer immunity. But, above all, fungi produce spores in the tissue, which are resistant to laser.
05.03.2021
From Saul to Paul
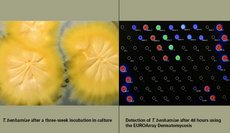
Mycology is one of the most beautiful faces of dermatology. To admire T. soudanense, T. violaceum or T. benhamiae in a Petri dish is an aesthetic enjoyment.